The Centers for Medicaid Services (CMS) is proposing to cut reimbursement for vascular access centers.
This could negatively impact dialysis patents’ access to care, which is why we have weighed in on this important issue.
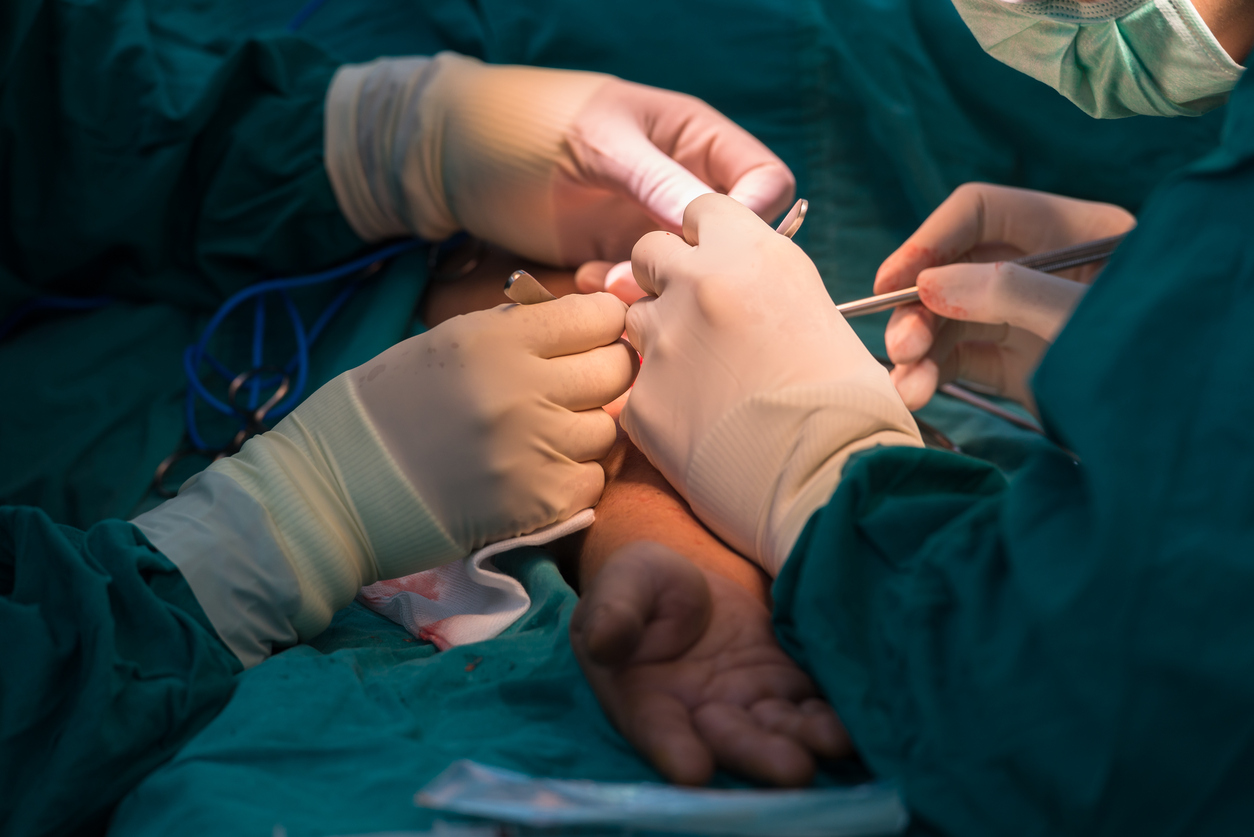
Dialysis Access and Fistulas
People with kidney failure need to have a dialysis access placed in order to receive live-saving dialysis treatments. Vascular surgeons create and maintain arteriovenous fistulas, which is a type of dialysis access. Fistulas are important for individuals on dialysis as they are considered a best practice in kidney care, improve patient outcomes and reduce the risk of infection.
Read DPC’s comment letter to CMS for additional information on this serious matter:
Seema Verma, Administrator
Centers for Medicare & Medicaid Services
200 Independence Avenue, SW
Washington, DC 20201
Re: CMS-1695-P – Revisions to Payment Policies under the Outpatient Prospective Payment System (OPPS) for CY 2019 Relating to Fees for Vascular Access Surgery Delivered to Dialysis Patients
Dear Administrator Verma:
Dialysis Patient Citizens (DPC) writes to offer its comments on the above referenced payment rules. DPC’s membership, currently 32,000, is restricted to kidney disease patients and their family members. DPC is a patient-led organization. Our by-laws require that the President, Vice President and at least 51% of the Board be current dialysis patients. For the past several years, the non-dialysis patients serving on the Board have been former dialysis patients with kidney transplants. Most of our volunteer board members have represented their peers on CMS technical expert panels and/or advisory committees of other health care organizations such as the National Quality Forum and Patient-Centered Outcomes Research Institute. DPC is committed to promoting access to high-quality dialysis care for individuals with ESRD; to prevention of, delayed onset of, and safe transition to ESRD among individuals with chronic kidney disease; and access to kidney transplantation as well as to other alternatives to dialysis that may emerge.
We are writing to express our opposition to what appears to be a 62% cut to reimbursements for vascular access surgery in the OPPS on top of a 39% cut that was made in the 2017 Physician Fee Schedule. We understand the importance, in a system of administered prices, of “getting the price right.” CMS should be vigilant to ensure that overpricing does not lead to overutilization, and that price differences, such as those relating to sites of care, do not create perverse incentives. What we do not understand is how the services of vascular surgeons who create and maintain A/V fistulas could fit in these categories. For dialysis patients, their vascular access site is a lifeline. These cuts represent a severe undervaluation of vascular access procedures relative to their importance to ESRD patients’ health.
Over a decade ago, CMS initiated a program called Fistula First to encourage the placement of A/V fistulas as access sites for dialysis. Fistulas are a much safer alternative to catheters, which are infection-prone. Infections from catheters not only threaten the well-being of dialysis patients but also impose the costs of complications on the Medicare program.
It is in the interests of both ESRD patients and the Medicare Trust Fund that there be easy availability of vascular surgeons to create fistulas in incident ESRD patients—ideally, before a CKD patient experiences complete kidney failure—and immediate availability of vascular surgeons when a fistula needs repair.
ESRD patients are the least stable, and the most costly, in the immediate aftermath of kidney failure. Placement of a fistula in incident patients is considered a best practice, and important work has been underway to develop quality measures and new payment models (including one endorsed by the PTAC) to incentivize timely referral of such patients to vascular surgeons.
ESRD patients also face a potential cascade of complications when a fistula is blocked and needs repair. Earlier this year we met a dialysis patient who, while away from home on vacation, experienced a blocked fistula. Due to delays in providing care at a hospital emergency department, her dialysis treatments were delayed and she suffered the loss of eyesight in one eye and amputation of a foot.
In recent years, mortality and morbidity in the ESRD population has decreased, in no small part due to improved vascular access care. It is short-sighted to mechanistically apply formulas to reduce fees for care of proven value. And it is especially foolish to do so at this time, when new global payment models that encourage greater coordination of and accountability for care are flowering.
Currently, Medicare and several large commercial payers are implementing total cost of care (TCOC) payment models in which dialysis providers accept significant performance risk to keep ESRD patients stable and healthy. One of these models is CMMI’s ESRD Seamless Care Organization (ESCO) initiative. Some of the more successful ESCOs are actually bringing in vascular surgeons and vascular access centers as partners in these arrangements. Such partnerships demonstrate the importance that dialysis providers—especially once they assume accountability for TCOC—recognize in the accessibility of these practices. As ESCO partners, the vascular access centers receive bonuses for shared savings along with the dialysis clinics, nephrologists, and in some cases hospitals. The sum of these bonuses plus the fees ordinarily billed by the surgeons represents the true value of their services to the patients, to the ESCOs, and to the Medicare program.
We are concerned that cuts to vascular access centers’ and surgeons’ reimbursements will have a domino effect jeopardizing the ESCO program as well as prospective TCOC arrangements that we had hoped and expected to multiply when ESRD patients are permitted to enroll in Medicare Advantage plans a few years from now. Quite simply, if vascular surgeons switch to more lucrative types of work and dialysis clinics are unable to arrange procedures when necessary, resulting in complications for which the ESCO or similar entity is accountable; or are forced to pay higher hospital outpatient department fees when surgery is performed, dialysis providers are less likely to assume risk for TCOC and less likely to implement accompanying care coordination strategies for their patients.
In closing, I would refer you to these observations made in the United States Renal Data System’s summary of its 2017 annual data report:
- “Seventeen percent of patients used an arteriovenous fistula exclusively at dialysis initiation. This increased to 65 percent by the end of one year on hemodialysis, and to 72 percent at the end of two years.
- “Eighty percent of patients still use catheters as the main vascular access at initiation of hemodialysis. This must change, as catheters predispose to serious infections and higher mortality.
- “Between 2001 and 2015, adjusted mortality rates decreased by 28 percent for dialysis patients. The net reductions in mortality from 2001 to 2015 were 27 percent for hemodialysis patients and 41 percent for peritoneal dialysis patients. However, since there appears to be a stabilization in mortality rates in recent years, there is no room for complacency.”
In our view, these cuts to reimbursement for vascular access surgery represent exactly the type of complacency that USRDS warned against. One can draw a straight line from the increased use of fistulas to the gains in patient lifespan. As USRDS noted however, the principal challenge to ESRD patients’ wellbeing is unacceptably high use of catheters at initiation of dialysis. Many stakeholders are committed, and many initiatives are underway, to address this problem; yet the OPPS rule is pulling in the opposite direction. We ask that you preserve the gains that have been made, and safeguard improvements in the pipeline, by ensuring patients’ continued access to vascular surgery.
Thank you for your consideration of our comments and concerns. If you have any questions or would like additional information, please do not hesitate to contact me or our Government Affairs Director Jackson Williams.
Sincerely,
Hrant Jamgochian, J.D., LL.M.
Executive Director