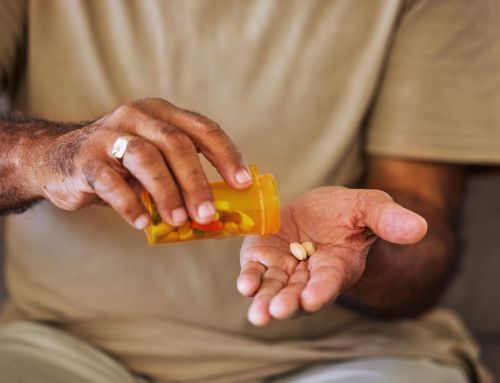
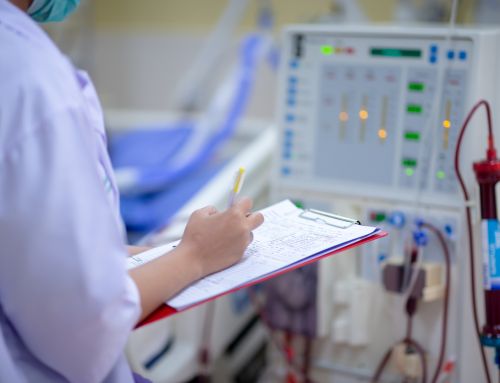
In 2021 End-Stage Renal Disease (ESRD) patients will be permitted to enroll in Medicare Advantage (MA) plans, potentially bringing major changes to ESRD care and how patients experience it. When open enrollment begins this fall, we want to make sure patients have access to the same robust benefits offered with MA plans right now. DPC reached out to the Centers for Medicare & Medicaid Services (CMS) with recommendations on how to ensure ESRD patients maintain the access, choice and quality care they expect when these benefits are available to everyone.
Currently, the only ESRD patients with MA plans are those whose kidneys failed while they were already enrolled in a plan. Starting in 2021, any ESRD patient will be able to switch to a MA plan if they choose to do so.
Read DPC’s full letter to CMS below:
Seema Verma, Administrator
Centers for Medicare & Medicaid Services
200 Independence Avenue, SW
Washington, DC 20201
Re: CMS-4190-P
Dear Administrator Verma:
Dialysis Patient Citizens (DPC) writes to offer its comments on the above referenced proposed rule relating to the Medicare Advantage program.
DPC’s membership, currently 32,000, is restricted to kidney disease patients and their family members. DPC is a patient-led organization. Our by-laws require that the President, Vice President and at least 51% of the Board be current dialysis patients. The non-dialysis patients serving on our Board are former dialysis patients with kidney transplants. Nearly all our volunteer board members have represented their peers on CMS technical expert panels and/or advisory committees of other health care organizations such as the National Quality Forum and Patient-Centered Outcomes Research Institute. DPC also conducts an Annual Membership Survey to ascertain patients’ experiences with their care and views on health policy issues. DPC is committed to promoting access to high-quality dialysis care for individuals with ESRD; to prevention of, delayed onset of, and safe transition to ESRD among individuals with chronic kidney disease; and access to kidney transplantation as well as to other alternatives to dialysis that may emerge.
Congress passed the ESRD Choice Act because of the likelihood that this complex and vulnerable population will have better outcomes if their care is coordinated through a Part C plan. While DPC takes no position on whether dialysis patients ought to enroll in MA plans, we believe they are likely to have improved outcomes if enrolled in a plan that uses a care delivery model such as that of successful ESRD Special Needs Plans (C-SNPs),1 the ESRD Seamless Care Organizations (ESCOs),2 or the Highmark-Davita partnership recounted in the April 2018 issue of the American Journal of Managed Care (AJMC).3 In all of these models, providers were held accountable for the total cost of care and used case management and other techniques to avoid complications. Most relevant here is the shared savings arrangement contracted between Highmark and Davita, described in the AJMC article, which led to dramatically reduced hospital admissions and length of stay for covered patients, including both commercial and MA enrollees. Implementation of the ESRD Choice Act holds the promise of considerable health gains to the ESRD population, but potential gains could be lost if the transition is mishandled.
Concerns About ESRD Payment Adequacy Could Fuel Risk Selection By Plans
We are concerned by the recent move by Kaiser-Permanente to change the cost sharing structure for dialysis from zero co-pay to 20% cost sharing. We believe this reflects a worry on the part of MA plans that a favorable benefit structure for ESRD patients will result in the plan attracting a large share of ESRD enrollees, thereby leading to competitive disadvantage. Implementation of the ESRD Choice Act will fail unless plans that believe they can profit by serving, and reducing complications for, ESRD patients, or at the very least, will not be punished for undertaking good faith efforts. We believe there are at least three approaches the Agency could take to eliminate this dynamic.
But first, a word about cost sharing for dialysis. Cost sharing is intended to prevent consumers from over-utilizing health care services, but dialysis will not be over-utilized by an ESRD patient. There is no “moral hazard” rationale for charging coinsurance for dialysis. It is for that reason that, when MedPAC surveyed cost sharing structures for dialysis in MA plans in 2004, it found that over 60% of plans, serving 75% of enrollees, had zero copays for dialysis. Evaluations of the ESCO program and the ESRD C-SNP program have found that dialysis utilization actually increases in total-cost-of-care arrangements relative to FFS, either because providers are ensuring that patients never miss a regularly scheduled treatment, or are providing additional treatments when patients need more fluid removed. The additional dialysis expenditures are more than offset by resulting lower hospitalization costs.
For this reason, the alteration of cost sharing for dialysis by MA plans is pennywise and pound-foolish in the aggregate, yet an expected net loss on ESRD patients could quite rationally bring into play a perverse “shirk” response to this Prisoner’s Dilemma scenario by individual plans. The result will be poorer outcomes overall if plans aren’t incentivized to duplicate the successful care model of the ESCOs and SNPs.
The Agency’s first option is to ensure ESRD benchmark calculations reflect actual costs and offer accurate, adequate payment for this unique patient population. Two actions could help achieve a more appropriate level of payment: (1) incorporating the cost of care during year one for ESRD beneficiaries when calculating the ESRD benchmark, and (2) setting the rates at the county level rather than the state level. We realize that this could increase Medicare expenditures. But we think that additional spending here would buy improved outcomes for patients by making them more attractive to plans and by making plans more attractive to beneficiaries.
For a potential expenditure-neutral alternative, the Agency could implement an ESRD risk reallocation mechanism based on the ACA’s risk adjustment program for qualified health plans. Unlike MA risk adjustment, which is prospective, the ACA’s risk adjustment program is retrospective and results in relatively larger payments to plans offset by transfers from plans enrolling healthier consumers. CMS could designate a small percentage of capitation payments that would be withheld from plans enrolling a lower number of ESRD patients than expected and redistribute those funds to plans enrolling a higher number of ESRD patients than expected. As with ACA’s “Three Rs,” the purpose would be to incentivize plans to enroll otherwise costly patients. However, this proposed reconciliation would apply based only on whether the beneficiary has ESRD or not.
A third option would be to mandate zero cost sharing for dialysis across the board. This would ensure that all plans would be on an even footing in their plan offerings, and beneficiaries would have access to the optimal benefit structure most likely to duplicate the positive results achieved by C-SNPs and ESCOs. The drawback to this approach is that while it is beneficiary-friendly, plans enrolling a disproportionate share of ESRD patients could suffer relative to competitors. But it would permit plans to encourage patient adherence to dialysis without fear of attracting too many ESRD patients. Such a mandate would be consistent with the Agency’s interest in promoting value-based insurance design (VBID) principles.
Loosening of Network Adequacy Requirements Would Jeopardize Implementation
We vigorously oppose the request by plans to loosen network adequacy standards. We surmise that a major motivation for the plans to seek narrowing of these protections is revealed in the paragraph of the proposed rule following the network adequacy discussion, citing complaints of “provider consolidation” and “prices well above Medicare FFS rates.” Let us be clear here: while it may be true that providers can “leverage” network adequacy requirements, network adequacy is a critical beneficiary protection. In the context of dialysis treatments, which require a patient’s presence three times a week, travel time and distance limits extend patients’ lives. A 50-mile drive does not become shorter as the Herfindahl–Hirschman Index rises. As such, network adequacy requirements cannot be used as a “dial” to be adjusted up or down to influence provider reimbursement. Using it as such is to “kick the dog” to lash out at providers, and a federal court applying the Administrative Procedure Act would almost certainly strike down changes that lack a nexus to patient access-to-care needs.
Considering the inclusion of home dialysis programs only as sufficient to satisfy network adequacy would be a trojan horse for risk selection. Home patients have lower total costs of care, but it remains uncertain to what extent that is a result of the modality or of the underlying demographics of home patients. Home dialysis patients are disproportionately white and affluent—in short, less likely to be impacted by social determinants of health. According to Shen et al (2020) in-center patients are disproportionately black or Hispanic, more likely to live in an economically deprived zip code, more likely to be unemployed, and more likely to be uninsured or on Medicaid.4
In 2013, 2014, and 2015, DPC used its annual Member Surveys to explore patient experience with and views on home dialysis. Results were consistent from year to year. The bottom line is that the research identified two types of “gaps” of interest to policymakers: Gaps in the delivery system that inhibit uptake of home dialysis, and gaps in patient preferences for home versus in-center modalities. We believe the “delivery system gap” that retards uptake of home dialysis can be addressed through benign interventions by MA plans; while the “preference gap” must be respected by CMS to avoid restricting patients’ choices.
Exhibit 1 illustrates the gaps. We preface this discussion by noting that approximately 20% of survey respondents dialyzed at home. Exhibit 1 shows that about 21-23% of patients felt that they had never been meaningfully or actionably informed about the option to use home HD or PD. We believe this represents a delivery system failure. We presume that many if not most of this subpopulation unexpectedly “crashed into” dialysis, which would constitute an explanation, but not an excuse. Our survey findings are roughly in accord with those of Mehrotra et al who, framing their question differently, found that 66% of ESRD patients were not initially presented with peritoneal dialysis as an option, 88% were not initially presented with home hemodialysis as an option, and 74% were not initially presented with transplantation as an option.5 We know that MA plans do a better job at identifying latent chronic kidney disease and we expect they will continue to make efforts, such as those pioneered by Kaiser-Permanente,6 to educate CKD patients on home modalities prior to kidney failure, and expedite patients’ access to them.
Exhibit 3 shows another side of the “delivery system gap”: 9-10% of respondents say they would consider home HD if their facility had training or if their doctor ordered it. Similarly, Exhibit 5 shows that 5-6% of respondents say they would consider PD if their facility had training or if their doctor ordered it. MA plans are well positioned to ensure that these options are better presented to patients.
Turning back to Exhibit 1, the patient “preference gap” is illustrated by the difference in the proportion of patients who were informed about home modalities—71-73%—and those who seriously considered home modalities, 22% and 33% for HHD and PD, respectively. This gap of 40-49% represents patients who weighed the relative advantages of home versus in-center and struck the balance in favor of in-center. Exhibits 2 and 4 display the reasons these patients reached that conclusion. Note that patient preferences regarding safety and social considerations predominate.
In sum, we feel that an expectation that great numbers of patients would choose home dialysis such that network coverage of only home dialysis would suffice is completely unrealistic. The predictable result of limiting a network to home providers would be to deter enrollments. We also worry that this request by insurers raises the specter of “step therapy” for dialysis, by which patients would be forced to use and fail at home dialysis first.
As we have demonstrated with the survey data presented in our previous communications with the Agency, we think it is unlikely that dialysis patients will change clinics or nephrologists to join a Medicare Advantage plan. Practically speaking, for the goals of the ESRD Choice Act to be achieved, plans will have to literally meet patients where they are. We realize that this approach contradicts some principles of managed care network contracting and “managed competition,” but the circumstances of this transition are unique.
We do not know enough about Highmark-Davita partnership recounted in the American Journal of Managed Care to say whether it could or should be a template for paying for care of ESRD enrollees. But we can say that this is the outline of what we as patient advocates envisioned when we lobbied for the ESRD Choice Act. The Health Care Payment Learning & Action Network (HCPLAN), HHS’ public-private partnership to support linking healthcare payments to the value of care, set its goals for adoption of shared accountability alternative payment models for Medicare Advantage and traditional Medicare at 30 percent adoption by 2020, 50 percent by 2022, and 100 percent by 2025. While we’re not certain that the 100% goal can be met, we do think that HHS should aim for the first two goals in this MA ESRD transition, as this care model and payment model have proven themselves good for dialysis patients. Gutting network adequacy requirements would discourage the negotiations necessary to bring value- and outcome-based contracting on line.
The Highmark-Davita partnership also seems to us the outline of a sort of “grand bargain” between insurers and dialysis providers, in which insurers accept network adequacy requirements and market conditions as they are in exchange for dialysis providers accepting two-sided risk for the total cost of care of their patients. If negotiations need a nudge, the Agency could arrange mediation by a respected luminary—former HHS officials such as Andy Slavitt, Tom Scully, Mike Leavitt, and Kathleen Sebelius come to mind, as do academic figures such as John Rowe and Bob Kocher. We believe that foundation funding could probably be tapped to cover the costs of such mediation.
While we ask that HHS cultivate value-based arrangements, we realize that not all dialysis providers have the resources to take on insurance risk. We look forward to seeing how health plans’ existing case management infrastructure can be applied to ESRD patients, and how those resources might be deployed for patients treated by smaller, non-risk bearing dialysis organizations. It is important that MA plans bring the benefits of care coordination to all ESRD patients regardless of where they dialyze.
The approach of the first open enrollment period for Medicare ESRD beneficiaries is a critical moment for the Agency—an opportunity to scale up care coordination that must not be squandered. We ask that the Agency start with a vision of what coverage and care for dialysis patients should look like in 2021 and the years soon after, and work backwards from there to ensure that it is on track. While it is hard to project a normatively “correct” percentage of ESRD patients to enroll in MA, if it is much smaller than the 34% of beneficiaries who enroll overall, we would be concerned that this transition may have been botched. As stated above, we also believe that the percent of ESRD beneficiaries covered by value-based contracts with providers should be in the range of the HCPLAN goals of 30-50%, and that the Agency should do all it can to encourage such arrangements.
Thank you for your consideration of our comments and concerns. If you have any questions or would like additional information, please do not hesitate to contact me or our Vice-President of Public Policy, Jackson Williams.
Respectfully submitted,
Hrant Jamgochian, J.D., LL.M.
Chief Executive Officer