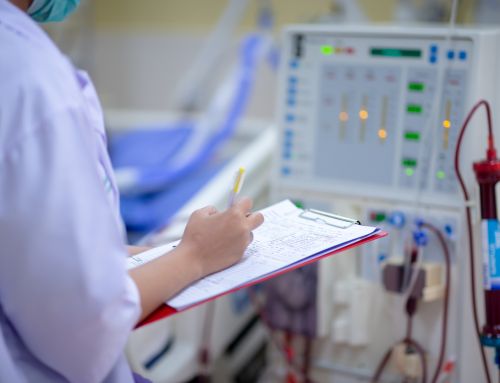
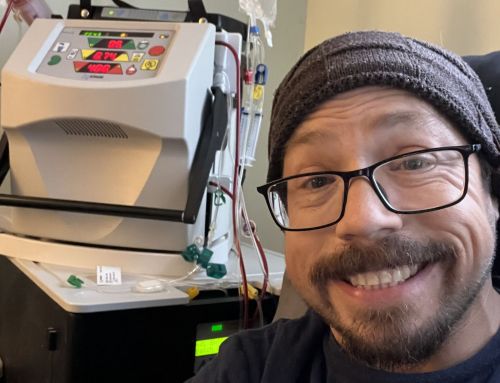
DPC Policy Director Jackson Williams and Pittsburgh kidney patient Janice Nathan were among witnesses at a hearing held by Pennsylvania’s insurance commissioner on “surprise medical bills.” These are bills received from physicians who are outside of an insurer’s provider network even though they work inside facilities that are in-network.
Janice Nathan’s primary care doctor recommended that she receive a cardiac stress test. Ms. Nathan checked her insurer’s provider directory and found an in-network facility to get the test. But when she received a cardiologist’s bill for $325—much more than the $50 co-pay she expected—she learned that the cardiologist who read the test results had not joined her insurer’s network.
DPC Policy Director Jackson Williams told the Commissioner, “The problem of surprise bills creates a dilemma for ESRD patients. Generally speaking, they prefer to keep their private insurance rather than switch to Medicare, as the actuarial value is richer, access to care is better, and satisfaction ratings are higher. Additionally, in the Exchange, low-income subsidies can be more generous than Medicare’s. But, out-of-network bills can quickly erode the financial advantages of private insurance. Dialysis patients should not have to be ducking crossfire between physicians and insurers as they try to cope with their kidney failure.”
The 2015 DPC Member Survey (sponsored by Abbott and Amgen) found that 30 percent of commercially insured dialysis patients received a surprise bill. Of those patients, 32 percent were charged an out-of-network rate by a provider they thought was in-network. These findings were almost a recent Consumers Union survey of commercially insured individuals, which found that patients who had been to a hospital during the past two years were more likely to receive such bills.