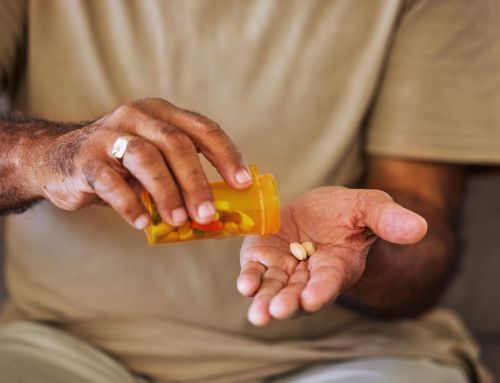
DPC provided feedback to the U.S. Department of Health and Human Services (HHS) regarding the COVID-19-related issues that the kidney community is facing. DPC made recommendations to HHS in the following areas:
- Transportation
- COVID-19 Treatments and Vaccinations
- Home Dialysis
People with End-Stage Renal Disease have a higher risk for developing a severe illness from COVID-19. As a result, it is crucial we do all that we can to help this vulnerable population in order to decrease the negative impact and spread of the virus.
Read DPC’s letter to HHS below for more details:
Kumiko Lippold, PhD, MPH
Department of Health and Human Services
330 C St SW
Washington, DC 20416
Dear Dr. Lippold,
In-center dialysis patients are uniquely vulnerable to this outbreak: like all kidney patients, they have weakened immune systems; and unlike many Americans who are able to remain safely confined at home, they must leave it three times each week to receive treatment in the company of other patients. While the medical advice given to most Americans is to stay at home, dialysis patients are urged in the strongest terms not to miss any treatments. Missed treatments can lead to a cascade of complications that add costs to the Medicare program.
Transportation
Funding Needed? Yes
Regulatory Change? Yes
Statutory Change? No
Our first request, therefore, is that Medicare assure that patients have access to transportation to their clinics. Many ESRD patients are dually eligible for Medicaid, and our member surveys indicate that about one fifth of patients receive non-emergency medical transportation (NEMT) to dialysis. But fee-for-service Medicare has no NEMT coverage.
We are concerned that this crisis could upend many patients’ usual transportation arrangements. First, many public transit systems are operating on reduced Sunday schedules. Since dialysis is not administered on Sundays, this presents patients with an unfamiliar, less convenient, and potentially inadequate option. Second, some dialysis facilities are expected to be designated as isolation units for patients who are infected. This means that both infected and uninfected patients may be directed to other facilities, based on whether the designation for their home facility matches their status. Finally, a patient who falls ill may be unable to drive to the facility, and patients regularly driven to a facility by a caregiver could lose their ride if their caregiver is ill or quarantined.
We urge CMS to use its demonstration authority to create a temporary billing code for NEMT for dialysis patients for the duration of this crisis. Medicare Administrative Contractors could make determinations as to eligibility on a case-by-case basis.
We also ask that dialysis providers be given relief from beneficiary inducement prohibitions if they are arranging transportation for patients who need it. We understand that some providers may already be arranging transportation in exigent circumstances, at their own expense; but we doubt that every provider has the resources to afford this, nor that even the largest providers could afford to do this indefinitely given their slim Medicare margins.
COVID-19 Treatments and Vaccinations
Funding Needed? No
Regulatory Change? No
Statutory Change? No
Our second request is that Medicare prioritize dialysis patients for any protective measures in short supply. Given ESRD patients’ vulnerability to communicable disease, personal protective equipment for clinic staff, any vaccine developed for COVID-19, and any treatments for COVID-19 will have maximum impact if first directed to this population.
Home Dialysis
Funding Needed? Yes
Regulatory Change? No
Statutory Change? No
Finally, this crisis demonstrates that the Administration was correct in making home dialysis uptake a policy priority. But the crisis also shows that CMS’ selection of a blunt, cost-cutting bonus-and-penalty payment adjustment to achieve this objective was short-sighted. A step CMS could take to have an immediate impact on home dialysis use would be to commit Innovation Center funding for staff-assisted home dialysis and urgent-start peritoneal dialysis programs. Demonstrations of these techniques should replace the flawed ETC demonstration proposed last year.
Thank you for your consideration of our comments and concerns. If you have any questions or would like additional information, please do not hesitate to contact me or our Vice-President of Public Policy, Jackson Williams.
Respectfully submitted,
Hrant Jamgochian, J.D., LL.M.
Chief Executive Officer