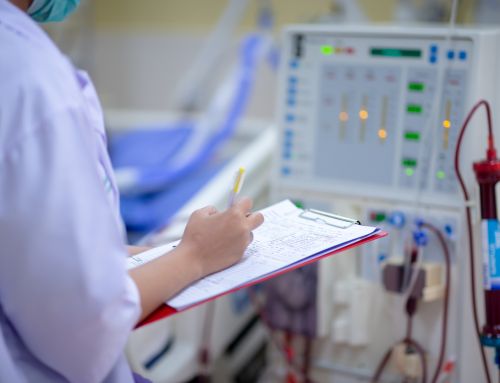
Receiving dialysis treatment three times a week is critical to survival for the 70,000 patients in California with End-Stage Renal Disease, or kidney failure.
Unfortunately, this access to treatment is being threatened with California Assembly Bill 290 (Woods), which may disrupt the provider network dialysis patients rely on and lower the quality of care they depend on. This legislation is similar to Senate Bill 1156, which was defeated by dialysis patients and vetoed by California Governor Jerry Brown last year.
Specifically, we are concerned that AB 290 will cut reimbursement rates private insurance companies pay to cover dialysis care. These reimbursement rates are crucial to dialysis facilities because Medicare does not cover the full cost of care for treating dialysis patients.
Reduced payments may force numerous facility closures, especially in rural and underserved areas. As a result, many patients will be required to find new dialysis centers, some of which will be much further away from their current facility. In addition, less money will be available for dialysis providers to donate to patients that rely on charitable assistance, which helps patients better afford their healthcare costs.
Encourage your California peers to take action.